Pregnancy and Periodontitis: Key Insights into Their Correlation

Pregnancy and Periodontitis: Key Insights into Their Correlation – Every form of life thrives to exist forever and the essence of human existence lies in the potentiality of reproduction. The responsibility of this power of creation has been granted largely to women. Every conception brings along exuberant excitement and joy but where there is light there is shadow too.
Since it is no point questioning the universe for the coexistence of good with evil, lets only learn to deal with the consequences of the good. Every pregnancy is unique and a woman’s body goes through tremendous hormonal and physiological changes throughout the process. This article discusses ramifications of only the oral cavity which might be encountered during the gestation period.
Oral issues associated with pregnancy are: Pregnancy/gestational gingivitis, pregnancy tumours, Xerostomia, Halitosis, caries, tooth sensitivity etc.

Gingivitis
Prevalence of Gingival issues are common during pregnancy. Although etiology is to be further explored, it is known to be caused due to raised hormonal levels which impact the periodontal structures. Two major hormones which increase dramatically are Oestrogen and Progesterone. Gingivitis is very common during pregnancy as more than 50% of pregnant women experience it. Gingivitis is a primary phase and is often followed by periodontitis if left unattended. Fluctuation in hormones is another cause of its aggravation. The process could eventually impact other supporting structures around the tooth too which involve bone crestal height and density.
Bleeding of gums is another salient feature which is not only evident to the dental surgeon but also to the patient. Vascular permeability of gingiva gets elevated during pregnancy hence chances of inflammations also rise. If there is marked gingivitis, either due to pregnancy or due to underlying cause before pregnancy, gums bleed during eating or brushing teeth. This is primarily a reason which urges the patient to reach out to a dentist.
Prominent signs of gingivitis: Bleeding while brushing or flossing, pain/tenderness in gums, redness, swelling/puffiness in gums, receding gums, tooth mobility and sensitivity to hot and cold.
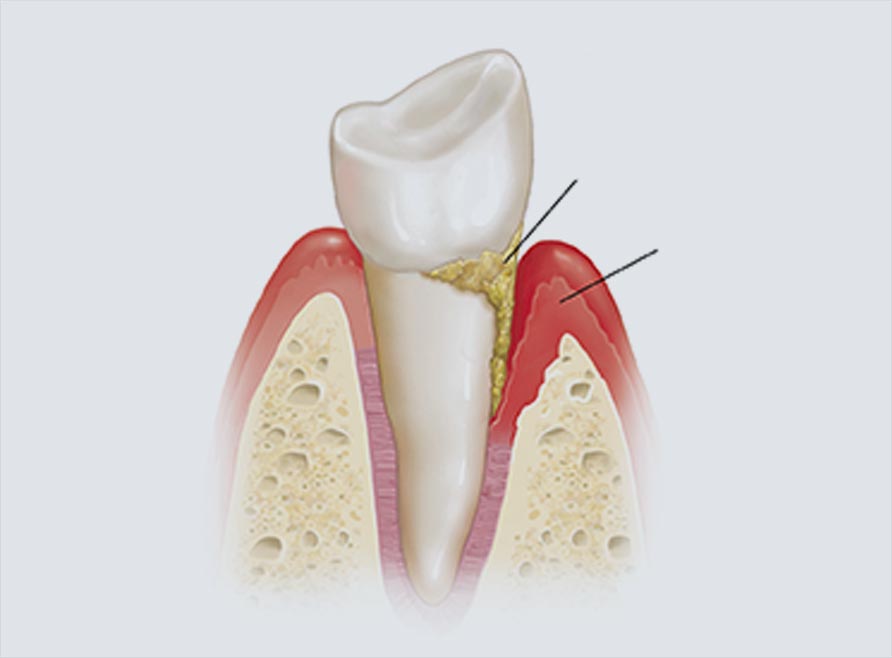
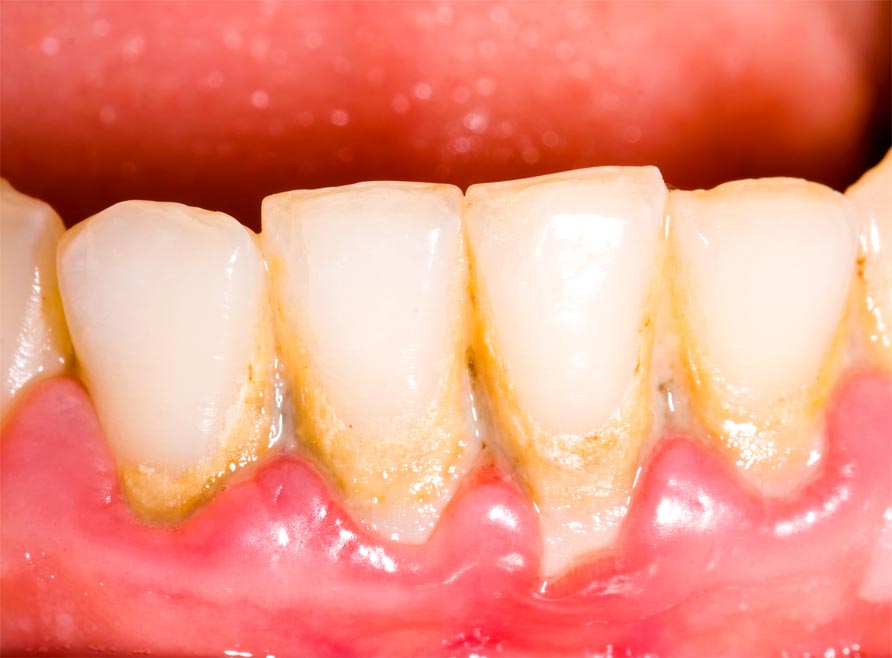
Periodontitis
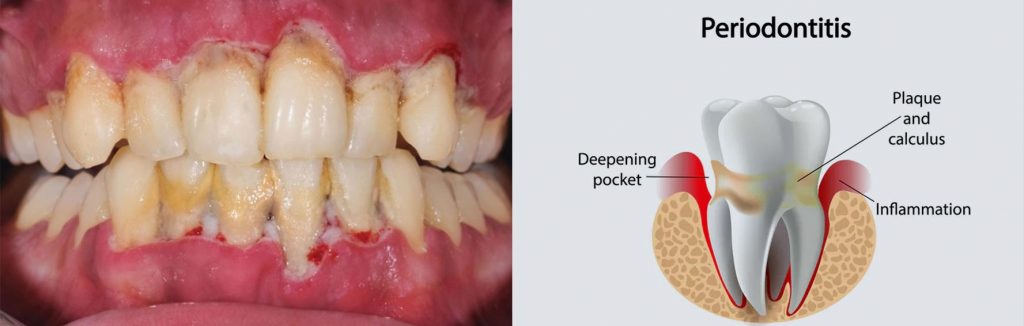
If Gingivitis gets worse it is followed by Periodontitis which impacts bone surrounding the teeth. Periodontitis is a prominent condition which is associated with excessive redness, swelling, bleeding gums, sensitivity to extreme temperatures, calculus accumulation, bone resorption etc. In worst scenario where these signs are ignored, periodontitis is accompanied with mobility of teeth and might even lead to extraction of the affected ones. Periodontitis is not just harmful for mouth but also could harm pregnancy and baby’s health. It must not be ignored or taken lightly as it could cause low birth weight of the child or a pre-term birth.
Pregnancy tumours
In some cases, a large reddish lump surrounded by inflamed gum tissue usually appears at the interdental gingival papilla which is referred to as pregnancy tumour. It is painful and causes discomfort in eating and speaking. Pregnancy tumours are mostly seen during the second trimester and is a pathology which typically occurs where pregnancy gingivitis is notable. This tumour is benign in nature so does not spread, nor is cancerous. Although it is not a lesion which would last for a long time but has to be removed in some cases where it creates functional problems. In other cases, they disappear after the child’s birth. The surgeon decides to surgically excise the tumour only if it is problematic as it may reoccur after removal. It is always wise to keep a check on the underlying causes to keep plaque accumulation under control. Basic daily oral hygiene and regular oral prophylaxis could largely reduce the chances of its occurrence.
Pregnancy tumour has many other pathological names like lobular capillary hemangioma, pregnancy epulides, Epulis Gravidarum, granuloma of pregnancy and pyogenic granuloma.

Gestational Diabetes
Pregnancy might also give rise to gestational diabetes which leads to elevated glucose levels in blood and thereby affecting oral tissues as well. Increase in the level of oral fauna, triggered by gestational diabetes becomes another predisposing factor for gingivitis. Gums become vulnerable to plaque deposition which is a beginning of series of gum issues.
Many studies have found an association between Gestational Diabetes Mellitus (GDM) and Gingivitis/periodontal issues. If one theory argues that GDM leads to periodontitis, the other asserts that periodontitis gives rise to Gestational diabetes. More profoundly accepted hypothesis is that periodontal disease is a risk factor which could result in pregnancy diabetes. This certainly infers that both are interlinked and must not be overlooked as they may cause foetal complications and could also harm the mother. Pregnant women with GDM are at higher risk of complications like preeclampsia and foetal complications like neonatal hyperglycaemia, foetal macrosomia or shoulder dystocia.
Further progressive research and study is required to substantiate both the factors and their interdependence.
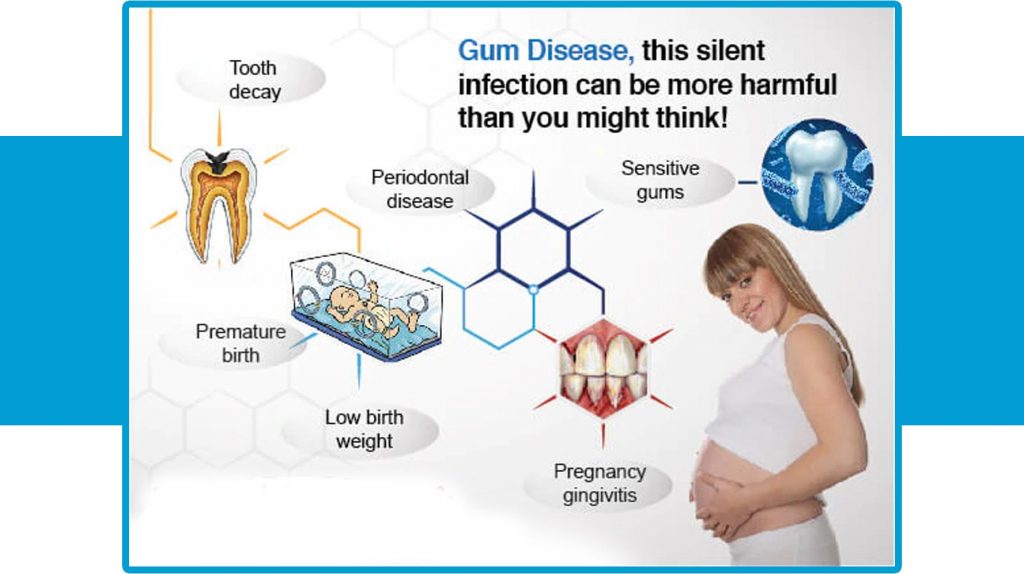
Caries
Poor oral hygiene or inability to maintain proper oral hygiene is the main cause of dental caries during pregnancy.
Prevention & Treatment
Prevention should remain the preferable course of action. Following given below things by a pregnant woman could minimize pregnancy-related dental concerns to a major extent:
- Brushing twice with right brushing technique using a fluoride toothpaste
- Switch to a soft toothbrush if regular one hurts/irritates/causes bleeding
- Flossing after meals – get rid of food lodgment
- Diet – avoid sugary drinks, avoid acidic foods, no smoking, no starchy foods
- Warm saline rinses (to keep inflammation at bay)
- Oral prophylaxis
- Antimicrobial mouth rinse
- Visit to the dentist at regular intervals
- Well-timed appointment – Impact begins in second month of pregnancy so scheduling an appointment at the right time is essential, as it gets worse until third trimester
- Keep a track of signs to be discussed with the dentist – red, swollen or bleeding gums, bad breath, difficulty in chewing food, pus discharge etc.
- Avoid over-indulgence into brushing or flossing – it might worsen the problems
- Healthy diet – whole grains, fruits, vegetables, dairy products
- Intake of foods containing calcium, Vitamin D, vitamin A and vitamin C

An interesting fact is the superstition revolving this idea which sometimes worsen the condition. A tradition running generation after generation misleads the pregnant woman to avoid brushing her teeth during a particular time period which hampers oral hygiene extensively and could bring about long-term harm or even irreversible damages.

A predisposing factor could be pre-existing periodontal problems which might be mistaken as solely the result of pregnancy. Hence, there is a need to do further research and studies to differentiate and demarcate impact on periodontium caused entirely by pregnancy.
Any oral pathology is an outcome of host’s response to the microbes which in turn leads to inflammatory reactions in form of gingivitis, periodontitis or other oral lesions. Changes in microbial profile at subgingival level is yet to be understood fully to reach a conclusion to this debate.
Studies show impact on Gingival index (GI), Plaque index (PI), Periodontal pocket depth (PPD) in pregnant women as compared to non-pregnant women. While plaque index (PI) remained similar, GI and PPD was noted significantly raised among pregnant women. Along with sex hormones – Oestrogen and Progesterone, GI and PPD were recorded again to normal levels after three months of childbirth which brings down the increased risk to dental issues discussed above.
The above said were some of the issues majorly addressed and known to occur during pregnancy, there are many other adverse effects still to be studied and emancipated to become familiar with.

No Comment